Hip Osteoarthritis: Causes, Symptoms, Treatment, and Prevention
What is Hip Osteoarthritis?
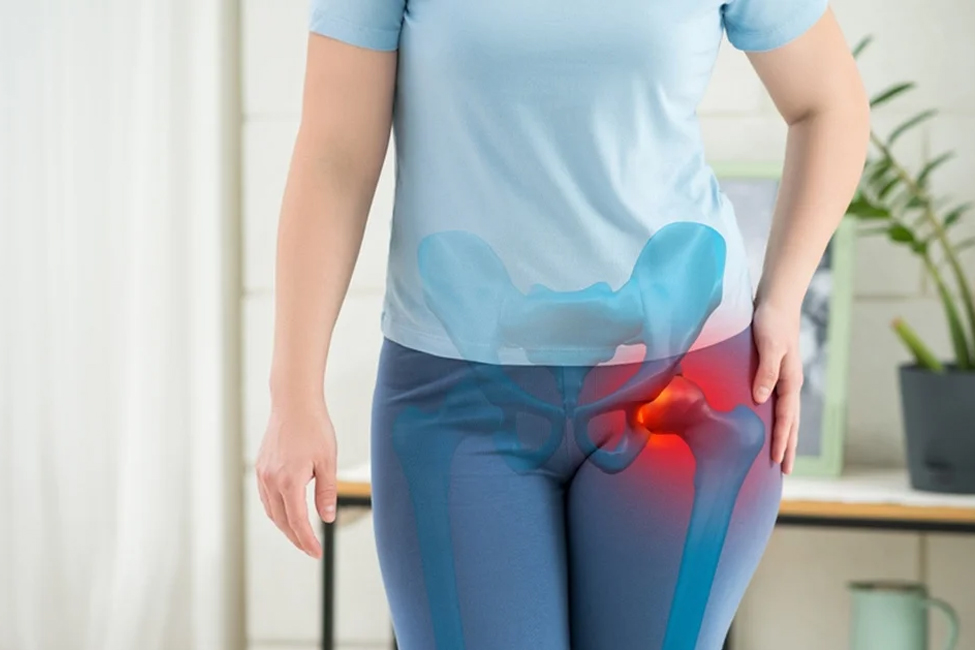
Hip osteoarthritis is a degenerative joint condition in the hip, where the cartilage covering the ends of the bones deteriorates, leading to pain, stiffness, and reduced mobility.
Types of Hip Osteoarthritis
Hip osteoarthritis can be broadly categorised into two main types based on its origins and development:
How Common is Hip Osteoarthritis?
Hip osteoarthritis is a prevalent condition, especially among older adults. It’s one of the most common forms of arthritis, with estimates indicating a significant portion of the population experiences hip osteoarthritis symptoms, particularly as they age.
Causes of Hip Osteoarthritis
The causes of hip osteoarthritis can be attributed to various factors:
- Age: The primary cause of hip osteoarthritis is the natural ageing process. Over time, the joint cartilage naturally deteriorates, impacting the hip joint’s ability to function properly.
- Joint Wear and Tear: Continuous use and repetitive stress on the hip joint due to regular activities or certain occupations can contribute to the breakdown of cartilage.
- Previous Injuries: Hip injuries or trauma, such as fractures or dislocations, can increase the likelihood of developing osteoarthritis in the hip joint later in life.
- Genetic Predisposition: Genetic factors might make certain individuals more susceptible to developing osteoarthritis due to inherent structural issues or tendencies toward joint degeneration.
- Joint Abnormalities or Conditions: Congenital hip abnormalities or developmental disorders affecting the hip joint’s structure might increase the risk of osteoarthritis.
- Obesity: Excessive weight can place additional stress on the hip joint, accelerating wear and tear and leading to a higher risk of osteoarthritis development.
Symptoms of Hip Osteoarthritis
Symptoms of hip osteoarthritis often include:
- Pain: Persistent or intermittent pain in the hip or groin area, which might worsen during movement or weight-bearing activities. The pain can range from a dull ache to sharp, shooting discomfort.
- Stiffness: Reduced range of motion in the hip joint, leading to stiffness, particularly after periods of inactivity or prolonged sitting.
- Decreased Mobility: Difficulty walking, climbing stairs, or performing daily activities due to pain and stiffness in the hip joint.
- Joint Instability: Some individuals might experience a feeling of joint instability or weakness in the affected hip.
- Audible Sounds: Clicking, popping, or grinding sensations (crepitus) within the hip joint during movement.
Diagnosis of Hip Osteoarthritis
Diagnosing hip osteoarthritis typically involves a combination of methods:
Medical History and Physical Examination
The orthopaedic specilialist will inquire about symptoms and medical history and perform a physical examination, evaluating range of motion, joint stability, and signs of discomfort.
Imaging Tests
Various imaging techniques help confirm the diagnosis and assess the extent of joint damage:
- X-rays: Provide detailed images of the hip joint, showing changes in bone structure and joint space narrowing associated with osteoarthritis.
- MRI (Magnetic Resonance Imaging): Offers detailed images of soft tissues, including cartilage, to assess the severity of joint damage.
- Blood Tests: While not specifically for diagnosing osteoarthritis, blood tests may be done to rule out other conditions or inflammatory joint diseases.
Diagnostic Injections
In some cases, an injection of a local anaesthetic into the hip joint may be used to confirm whether the pain originates from the hip joint itself, helping in the diagnosis.
Complications of Hip Osteoarthritis
Complications associated with hip osteoarthritis can include:
- Chronic Pain: Ongoing discomfort in the hip joint, affecting mobility and quality of life, can lead to chronic pain and decreased functionality.
- Functional Limitations: Severe hip osteoarthritis may significantly limit an individual’s ability to perform daily activities, affecting independence and quality of life.
- Joint Deformity: In advanced cases, joint deformity or bone spurs might develop, further impacting joint function and causing increased pain.
- Reduced Mobility and Independence: Severe osteoarthritis can lead to decreased mobility, requiring assistive devices or modifications to maintain independence.
- Secondary Health Issues: Mobility limitations can contribute to secondary health concerns such as weight gain, reduced physical activity, and associated health issues.
Treatment Options for Hip Osteoarthritis
Treatment options for hip osteoarthritis may include both non-surgical and surgical approaches:
Non-surgical Treatments
- Lifestyle Modifications: Adjusting activities to reduce stress on the hip joint.
- Physical Therapy: Engaging in exercises to strengthen hip muscles and improve joint flexibility.
- Medications: Pain relievers or anti-inflammatory medications to manage discomfort.
- Assistive Devices: Using canes or other devices to reduce joint stress.
Surgical Interventions
- Hip Arthroscopy: A minimally invasive procedure to address mild to moderate osteoarthritis by removing damaged tissue or bone spurs.
- Osteotomy: Surgical realignment of the hip joint to redistribute weight and reduce pressure on the damaged area.
- Total Hip Replacement (THR): In severe cases, replacing the damaged hip joint with an artificial one to improve mobility and reduce pain.
Preventing Hip Osteoarthritis
Preventing hip osteoarthritis involves various strategies to promote joint health and reduce the risk of degeneration:
- Managing body weight helps reduce stress on the hip joint, decreasing the risk of osteoarthritis development or progression.
- Engage in activities that strengthen hip-supporting muscles and promote joint flexibility, contributing to better joint health.
- Take precautions to prevent hip injuries, as previous injuries can increase the risk of developing osteoarthritis.
- Opt for low-impact exercises and activities that reduce stress on the hip joint, such as swimming, cycling, or walking.
- Practice correct posture and body mechanics to reduce unnecessary strain on the hip joint during daily activities.
- A balanced diet rich in nutrients, particularly those that support joint health, can aid in preventing osteoarthritis development.
Living with Hip Osteoarthritis
Living with hip osteoarthritis may involve several considerations to manage the condition and improve quality of life:
- Following the recommended treatment plan, including medications, physical therapy, and lifestyle adjustments, is crucial.
- Orthopaedic specialists recommend regular exercises to strengthen muscles and maintain joint flexibility.
- Using canes or other assistive devices to reduce joint stress and aid in mobility, if necessary.
- Maintaining a balanced diet, managing weight, and avoiding activities exacerbate hip discomfort.
- Attending scheduled medical appointments for routine check-ups or to address changes in symptoms.
Hip osteoarthritis is a challenging condition affecting joint health, mobility, and daily comfort. Understanding its symptoms, causes, and available treatments is essential for effective management. Prevention, early diagnosis, and appropriate interventions play a significant role in mitigating its impact on one’s quality of life.
For personalised evaluation, expert guidance, and tailored treatments specific to hip osteoarthritis, consider seeking an appointment with The Orthopaedic Practice and Surgery Clinic. Their specialised team can offer individualised assessments and effective strategies to address hip joint concerns, ultimately improving joint health and enhancing your overall well-being.
Don’t let hip osteoarthritis limit your lifestyle—schedule an appointment today with The Orthopaedic Practice and Surgery Clinic for specialised care and guidance tailored to your joint health needs.