Degenerative Disc Disease: Causes, Symptoms, Treatment, and Prevention
What is Degenerative Disc Disease?
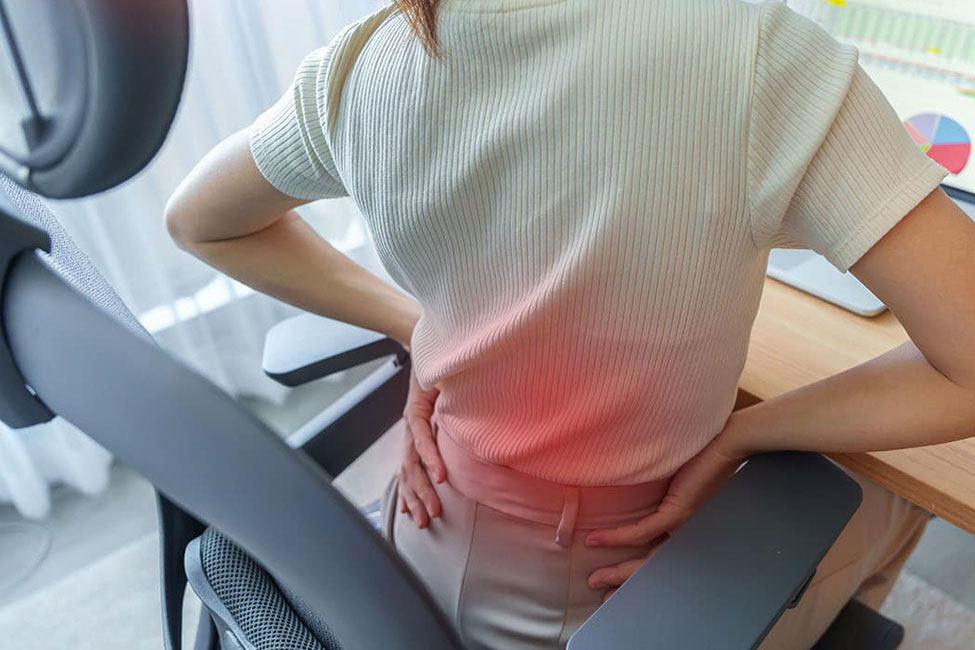
Degenerative Disc Disease is when the soft, cushion-like discs between the bones of your spine (vertebrae) wear down or degenerate over time. These discs act as shock absorbers and help your spine stay flexible. When they deteriorate, it can lead to pain and discomfort in the back and neck.
Types of Degenerative Disc Diseases
Degenerative Disc Disease typically refers to the general condition of spinal disc deterioration rather than specific “types” like other diseases. However, it can manifest in a few ways:
Disc Desiccation: This is when the discs lose moisture and become dehydrated, making them less effective as cushions between the vertebrae.
Disc Herniation: In this case, the disc’s inner material can bulge or rupture through the outer layer, potentially compressing nearby nerves and causing pain.
Spinal Stenosis: Degenerative changes in the discs can lead to a narrowing of the spinal canal, which can put pressure on the spinal cord and nerves, resulting in various symptoms, including pain and numbness.
While these aren’t distinct “types” of Degenerative Disc Disease, they represent different ways the condition can impact the spine and cause symptoms. The specific symptoms and treatments may vary depending on how these changes affect an individual’s spine.
How Common is Degenerative Disc Disease?
Degenerative Disc Disease is quite common, especially as people get older. Most of us will experience some degree of disc degeneration as we age. It’s one of the leading causes of back and neck pain. However, not everyone with disc degeneration experiences pain, and many can manage their symptoms with treatments like physical therapy or medication.
Causes of Degenerative Disc Disease
Degenerative Disc Disease is primarily caused by the natural aging process and wear and tear on the spine over time. Here are some of the key factors contributing to the development of this condition:
- Age: The most common cause. As we age, the discs in our spine gradually lose their ability to retain water and become less flexible, leading to degeneration.
- Genetics: Some individuals may inherit a predisposition for degenerative changes in their discs, making them more susceptible to the condition.
- Daily Wear and Tear: Repetitive movements, heavy lifting, poor posture, and physical strain over the years can contribute to disc degeneration.
- Smoking: Smoking reduces the blood supply to the discs, weakening them and accelerating degeneration.
- Injury or Trauma: A significant injury, such as a car accident or a fall, can damage the discs and accelerate their degeneration.
- Occupation: Certain jobs that involve heavy lifting, constant bending, or twisting can increase the risk of degenerative disc disease.
- Obesity: Excess body weight stresses the spine and can lead to more rapid disc degeneration.
Symptoms of Degenerative Disc Disease
Degenerative Disc Disease can cause various symptoms, ranging from mild discomfort to severe pain. These symptoms often result from the changes in the spinal discs and their impact on nearby structures like nerves. Common symptoms include:
- Back or Neck Pain: Persistent, aching discomfort in the lower back (lumbar region) or neck. The pain may come and go or be constant.
- Radiating Pain: Pain that extends into the arms or legs, depending on the location of the affected discs. This is often referred to as radiculopathy or sciatica.
- Numbness and Tingling: You may experience numbness, tingling, or a “pins and needles” feeling in the limbs due to nerve compression.
- Muscle Weakness: Weakness in the muscles of the legs or arms, which can make it difficult to perform everyday activities.
- Pain Aggravated by Movement: Pain worsens when you bend, lift, twist, or sit for prolonged periods. It may feel better when you change positions or lie down.
- Stiffness: A sense of stiffness in the spine, which can be more pronounced in the morning or after long periods of inactivity.
- Difficulty Walking: Severe cases may lead to difficulty walking, balance problems, or trouble with fine motor skills in the hands.
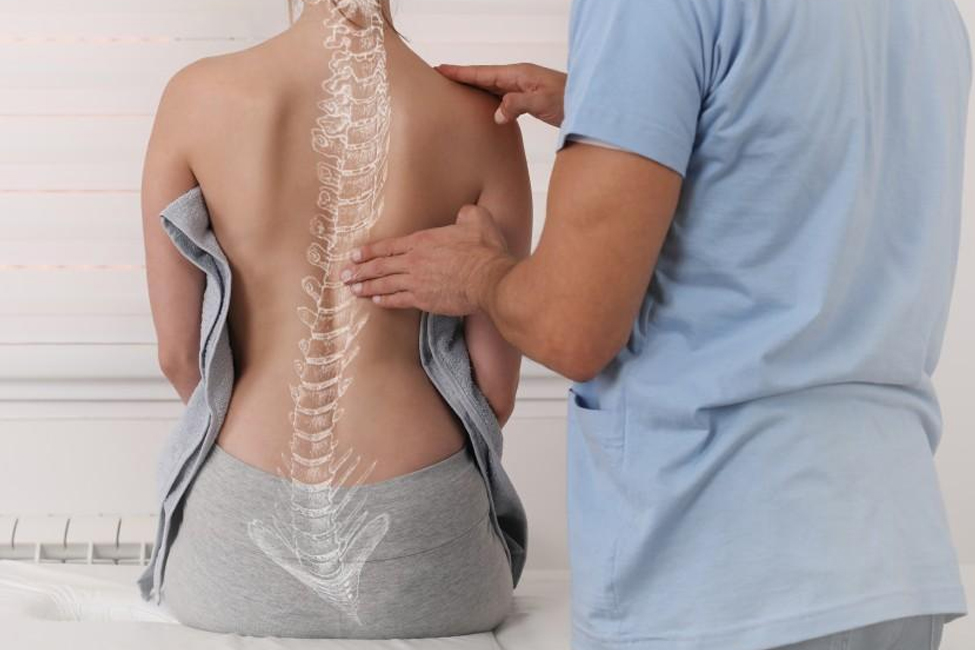
Diagnosis of Degenerative Disc Disease
Diagnosing Degenerative Disc Disease typically involves a combination of medical history, physical examination, and imaging tests. Here’s an overview of the diagnostic process:
Medical History
Your orthopaedic specialist will ask about your symptoms, including the type, duration, and location of pain or discomfort. They will also inquire about your daily activities, lifestyle, and any previous injuries or conditions related to your spine.
Physical Examination
The doctor will conduct a physical examination to assess your range of motion, muscle strength, reflexes, and nerve irritation or compression signs.
Imaging Studies
- X-rays: X-rays can provide a basic view of the spine’s alignment and any disc changes, such as narrowing or bone spurs.
- MRI (Magnetic Resonance Imaging): MRI scans offer detailed images of the spine and can show the condition of the discs, including their hydration and any herniation.
- CT (Computed Tomography) Scan: A CT scan is sometimes used to obtain more detailed images of the spine and discs, especially when a surgical approach is being considered.
Discography
In some cases, a discography may be performed. This involves injecting a contrast dye into the suspected degenerated disc to help pinpoint the exact source of pain. It’s often used when the diagnosis is unclear from other imaging studies.
Nerve Conduction Studies
If there are signs of nerve compression or radiculopathy, nerve conduction studies or electromyography (EMG) may be performed to assess nerve function.
Bone Scans
Occasionally, bone scans may rule out other bone-related conditions or identify areas of increased bone activity.
Blood Tests
Blood tests are typically not used to diagnose Degenerative Disc Disease but may be conducted to rule out other potential causes of symptoms, such as infections or inflammatory conditions.
Complications of Degenerative Disc Disease
Degenerative Disc Disease is not typically life-threatening, but it can lead to various complications and negatively impact a person’s quality of life. Some potential complications and associated issues include:
- Chronic Pain: Persistent back or neck pain can significantly reduce a person’s quality of life, limit their ability to perform daily activities, and lead to chronic discomfort.
- Nerve Compression: As the discs deteriorate, they can herniate or compress nearby nerves, causing radiating pain, numbness, and weakness. This can affect mobility and functionality.
- Reduced Mobility: Pain and stiffness in the spine may result in a reduced range of motion, making it difficult to bend, twist, or even walk comfortably.
- Muscle Weakness: Nerve compression can lead to limb muscle weakness, potentially affecting balance and coordination.
- Functional Limitations: Degenerative Disc Disease can hinder one’s ability to perform physical tasks, impacting job performance and activity participation.
- Mental Health Impacts: Chronic pain and reduced physical function can lead to depression, anxiety, and a decreased overall quality of life.
- Spinal Instability: In some cases, advanced disc degeneration can lead to spinal instability, which may necessitate surgical intervention to stabilise the spine.
- Increased Risk of Other Spinal Conditions: Degenerative Disc Disease may contribute to or increase the risk of other spinal conditions, such as spinal stenosis or facet joint arthritis.
- Reduced Quality of Life: Chronic pain and limitations in mobility and functionality can significantly impact a person’s overall well-being and quality of life.
Treatment Options for Degenerative Disc Disease
The choice of Degenerative Disc Disease (DDD) treatment depends on the severity of your symptoms and their impact on your daily life. Here are various treatment options to consider:
Conservative (Non-surgical) Treatments
- Pain Medication: Over-the-counter or prescription medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can help manage pain and inflammation.
- Physical Therapy: A physical therapist can create a customised exercise program to strengthen the back and core muscles, improve flexibility, and relieve pain.
- Lifestyle Modifications: Maintaining a healthy weight, proper ergonomics, and avoiding activities exacerbating your symptoms.
- Hot and Cold Therapy: Applying heat or cold to the affected area can help relieve pain and reduce muscle spasms.
- Epidural Steroid Injections: Injections of corticosteroids into the affected area can temporarily relieve pain and inflammation.
Minimally Invasive Procedures
- Radiofrequency Ablation: This procedure uses radio waves to heat and interrupt nerve signals in the affected area, reducing pain.
- Nucleoplasty: A minimally invasive procedure that uses radiofrequency energy to shrink and seal the damaged disc tissue.
- Laser Disc Decompression: A laser vaporises disc material and reduces nerve pressure.
Surgical Options
- Discectomy: In cases of severe pain or nerve compression, a surgeon may remove the damaged portion of a disc.
- Spinal Fusion: Fusion surgery stabilises the spine by joining two or more vertebrae together with the help of metal hardware. This is often considered for severe DDD or spinal instability.
- Artificial Disc Replacement: In this procedure, the damaged disc is replaced with an artificial one, preserving motion in the spine.
Regenerative Medicine
Emerging treatments like stem cell therapy and platelet-rich plasma (PRP) injections are being explored for their potential to promote disc healing and reduce pain.
Complementary Therapies
Some individuals find relief through therapies like acupuncture, massage, or yoga, which can help manage pain and improve overall well-being.
Preventing Degenerative Disc Disease
While Degenerative Disc Disease (DDD) is often a result of the natural ageing process, there are several lifestyle choices and habits that can potentially reduce the risk or slow down the progression of this condition:
- Excess body weight stresses the spine, accelerating disc degeneration. A balanced diet and regular exercise can help control weight.
- Engage in regular physical activity to keep your spine strong and flexible. Focus on exercises that promote core strength and good posture, like swimming, walking, and yoga, can be particularly beneficial.
- When lifting heavy objects, bend at the hips and knees, not at the waist, and use your legs to lift rather than your back.
- Ensure your workplace or home office is set up ergonomically. Use a chair with proper lumbar support and maintain good posture while working at a computer.
- Smoking reduces blood flow to the discs in the spine, making them more prone to degeneration. Quitting smoking can help prevent or slow DDD.
- Drink plenty of water to keep the spinal discs well-hydrated. Proper hydration is essential for maintaining disc health.
- Incorporate stretching into your daily routine to maintain flexibility in your spine and reduce the risk of stiffness.
- Be conscious of your posture, whether sitting or standing. Good posture can reduce the strain on your spine.
- Choose a mattress and pillows that provide good support for your spine. A medium-firm mattress is often a good choice.
- Keep up with routine medical check-ups to monitor your spine’s health and address any issues early.
Living with Degenerative Disc Disease
Living with Degenerative Disc Disease (DDD) can be challenging, but with the right strategies and support, you can manage your symptoms and maintain a good quality of life. Here are some tips for coping with DDD:
- Establish a relationship with healthcare professionals specialising in spine-related issues. They can help diagnose your condition, guide treatment options, and monitor your progress.
- Develop a pain management plan with your orthopaedic specialist. This may involve medications, physical therapy, or minimally invasive procedures to help alleviate discomfort.
- Engage in regular, low-impact exercise to strengthen your core muscles and improve flexibility. Consult a physical therapist for a customised exercise program that suits your condition.
- Maintain good posture and use proper body mechanics when lifting or performing daily tasks to reduce the strain on your spine.
- Ensure your workspace is ergonomically designed to support your spine, whether at work or home. Invest in a comfortable chair and set up your computer or desk to promote good posture.
- Maintain a healthy diet and manage your weight to reduce the strain on your spine. Consult a registered dietitian if necessary.
- If you smoke, consider quitting. Smoking reduces blood flow to the spine and can exacerbate DDD.
- Chronic pain can be emotionally taxing. Practice stress-reduction techniques such as meditation, deep breathing, or mindfulness to improve your mental well-being.
- Choose a mattress and pillows that provide good spinal support and comfort for a restful night’s sleep.
- Consider using assistive devices or supports like lumbar cushions or braces to reduce discomfort and strain during daily activities.
- Some individuals find relief through complementary therapies like acupuncture, massage, or chiropractic care. Consult with your orthopaedic specialist before trying these options.
- Be mindful of your activities, and pace yourself. Avoid activities that exacerbate your symptoms, and take breaks when needed.
- Regularly follow up with your orthopaedic specialist to assess your condition’s progression and adjust your treatment plan.
Your health and well-being are of utmost importance, and some medical professionals specialise in diagnosing and treating spine-related issues like DDD. Don’t hesitate to seek your help and support to lead a more comfortable and fulfilling life.
If you’d like to request an appointment with The Orthopaedic Practice and Surgery Clinic, a trusted provider with expertise in treating spine conditions, take that proactive step towards managing your DDD. Your spine health matters and professional guidance can significantly impact your journey to a healthier and happier life. Don’t wait – take action and prioritise your well-being today.