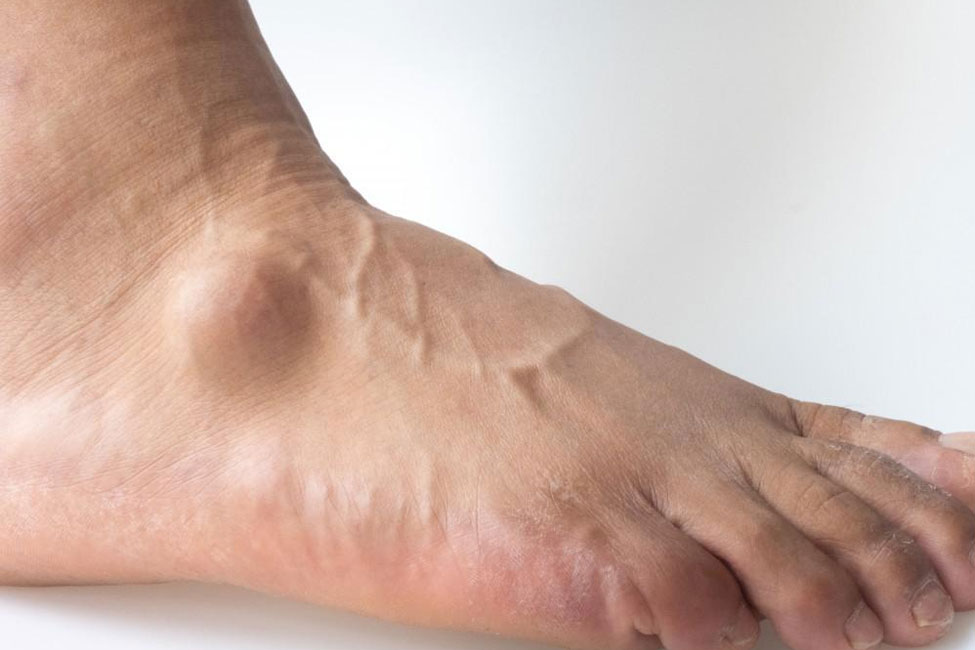
A ganglion cyst is a noncancerous, fluid-filled lump that often forms near joints or tendons. These cysts typically manifest as small, round sacs filled with a jelly-like fluid arising from the synovial lining of a joint or tendon sheath. While generally benign, they can cause discomfort and affect joint functionality.
Ganglion cysts frequently emerge in areas surrounding joints or tendons, with a notable prevalence in the wrists or hands. However, they can also occur in other locations, such as the ankles or feet. The cysts may vary in size, and their visibility can change over time.
Ganglion cysts frequently emerge in areas surrounding joints or tendons, with a notable prevalence in the wrists or hands. However, they can also occur in other locations, such as the ankles or feet. The cysts may vary in size, and their visibility can change over time.
Anatomy of a Ganglion Cyst
Ganglion cysts originate from the synovial lining of a joint or tendon sheath, accumulating a gelatinous fluid within the sac. This fluid is often viscous and clear, contributing to the cyst’s distinctive appearance.
Common Locations
Wrist and hand ganglion cysts – Ganglion cysts most frequently occur in the wrists and hands. The dorsal surface of the wrist, near the scapholunate ligament, is a common location. Additionally, ganglion cysts can appear on the palmar surface of the wrist, fingers, or the back of the hand. Their notable prevalence in these areas may be visible or palpable, depending on their size and depth.
Occurrence in other joints (knees, ankles) – While the wrists and hands are primary locations, ganglion cysts can also develop in other joints, such as the knees and ankles. In these instances, the cysts may emerge near the ligaments or tendon sheaths associated with these joints. Although less common in these areas, ganglion cysts can still pose similar challenges, impacting joint function and causing discomfort.
Causes and Risk Factors of Ganglion Cyst
The exact cause of ganglion cysts is not always clear, but several factors and risk factors may contribute to their development:
Overuse or repetitive activities
Ganglion cysts often develop due to overuse or repetitive activities that irritate the joints or tendon sheaths. These activities may include repetitive hand or wrist movements, leading to micro-trauma and irritation in the affected area.
Micro-trauma leading to cyst formation
Micro-trauma, resulting from repetitive stress or strain on a joint or tendon, can contribute to the formation of ganglion cysts. The cumulative effect of minor injuries or irritation may trigger the development of a fluid-filled sac, especially in areas prone to overuse.
Dysfunction in the joint or tendon sheath
Dysfunction in the joint or tendon sheath, often related to issues with the synovium, can lead to ganglion cyst formation. The synovium, responsible for producing synovial fluid to lubricate joints and tendons, may experience disruptions, causing an abnormal accumulation of fluid and subsequent cyst development.
Fluid accumulation causing cyst development
Ganglion cysts result from the abnormal accumulation of synovial fluid within the joint or tendon sheath. This fluid accumulation may occur due to various factors, such as joint or tendon sheath dysfunction, leading to the formation of a cyst as the fluid collects in a localised sac.
Higher prevalence in individuals aged 20 to 40
Ganglion cysts are more commonly observed in individuals aged 20 to 40. This age group tends to engage in activities that may contribute to joint or tendon irritation, increasing the likelihood of cyst development. The prevalence in this age range suggests a correlation between certain activities and the formation of ganglion cysts.
Occurrence more common in females
Ganglion cysts exhibit a higher occurrence in females compared to males. While the exact reasons for this gender difference are not fully understood, hormonal factors and variations in joint mechanics may play a role. Understanding the gender-related risk can aid in targeted prevention and management strategies.
Symptoms of Ganglion Cysts
Symptoms of ganglion cysts can vary from person to person, and not all individuals with ganglion cysts experience the same set of symptoms. The common symptoms associated with ganglion cysts include:
Visible Lump
Ganglion cysts typically manifest as a noticeable lump often round or oval in shape. The lump may be soft and may move slightly when touched.
The size of the cyst may change over time. It might fluctuate in size, appearing larger at times and smaller at other times. Factors like activity level and joint movement often influence changes in size.
Pain or Discomfort
Pain or discomfort may be experienced when the affected joint is moved or when pressure is applied to the cyst. The pain can range from mild to moderate and may be intermittent.
The degree of pain experienced can vary among individuals. Some people with ganglion cysts may not feel any pain, while others may experience significant discomfort.
Numbness or Tingling
In some cases, ganglion cysts may compress nearby nerves, leading to numbness or tingling sensations in the affected area. This can result in altered sensations in the fingers or hand if the cyst is near the wrist.
Individuals with ganglion cysts may report numbness, tingling, or a “pins and needles” sensation in the region where the cyst is located. This is particularly common when the cyst exerts pressure on nerves.
Diagnosis
The combination of clinical examination and imaging studies is often effective in diagnosing ganglion cysts. The clinical assessment helps determine the cyst’s impact on joint function and associated symptoms, while imaging studies provide detailed information about the cyst’s characteristics and location.
Clinical Examination
An orthopaedic specialist or a general practitioner will perform a thorough physical examination. This includes assessing the appearance, size, and consistency of the lump associated with the ganglion cyst.
The healthcare professional will examine the affected joint’s range of motion and assess any discomfort or pain associated with movement. This helps determine the impact of the cyst on joint function.
Imaging Studies
Ultrasound is a commonly used imaging technique to visualise ganglion cysts. It provides real-time images that allow the healthcare provider to observe the cyst’s size, location, and relationship with adjacent structures. Ultrasound is particularly useful for cysts near the surface of the skin.
An MRI may be recommended for a more detailed and comprehensive view of the ganglion cyst in some cases. MRI can provide high-resolution images that help assess the cyst’s internal structure, its relation to nearby tissues, and its impact on joint structures.
Treatment Options
Conservative treatments and surgical options offer a range of approaches for managing ganglion cysts based on the cyst’s characteristics, symptoms, and patient preferences. The choice of treatment is tailored to individual cases, with the goal of alleviating symptoms and preventing recurrence.
Conservative Treatments
Observation and Monitoring
- Asymptomatic ganglion cysts, those causing no pain or functional impairment, may be observed without immediate intervention. Regular monitoring through periodic check-ups allows healthcare professionals to track any changes in size or symptoms.
- Regular follow-up appointments are essential for monitoring asymptomatic cysts. Through clinical examination and, if necessary, imaging studies, healthcare providers can assess the cyst’s stability, growth, or potential resolution over time.
Immobilisation
- Immobilisation involves braces or splints to restrict joint movement, reducing stress on the affected area. This can alleviate irritation and potentially limit the size of the ganglion cyst by minimising movement-related fluid accumulation.
- Immobilisation aims to decrease joint or tendon irritation, reducing the ganglion cyst’s size. Limiting movement may shrink the cyst, and symptoms such as pain and discomfort may be alleviated.
Aspiration
- Aspiration involves using a needle to drain the fluid from the ganglion cyst. This procedure is performed under sterile conditions and may be an option for symptomatic cysts causing discomfort. Draining the fluid can provide temporary relief from pain and pressure.
- While aspiration can provide symptomatic relief, it is important to note that ganglion cysts may recur, necessitating additional procedures. The potential for recurrence should be discussed with the patient, and the decision to pursue aspiration should consider the cyst’s characteristics and the individual’s symptoms.
Surgical Options
Excision
- Excision involves completely removing the ganglion cyst, including its connection to the joint or tendon sheath. This surgical option is considered for persistent or symptomatic cysts that do not respond to conservative treatments.
- Excision procedures are often performed on an outpatient basis. The surgical intervention aims to eliminate the cyst and its connection to prevent recurrence, promoting long-term relief from symptoms.
Arthroscopy
- Arthroscopy is a minimally invasive surgical procedure involving a small camera (arthroscope) to visualise and access the joint. This technique allows for exploration and removal of the ganglion cyst while minimising trauma to surrounding tissues.
- Arthroscopy provides a detailed view of the joint, enabling surgeons to explore and remove the ganglion cyst. This approach often results in smaller incisions, reduced postoperative pain, and quicker recovery compared to traditional open surgery.
Recovery and Rehabilitation
Following surgical intervention for ganglion cysts, a structured rehabilitation timeline is established. Patients are provided with guidelines on activity restrictions during the initial recovery period. The rehabilitation plan is tailored to the individual’s specific case, considering factors such as the size and location of the cyst.
The recovery process involves a gradual return to normal activities. Physical therapists may prescribe specific exercises to improve joint mobility and strength. Patients are advised to follow the recommended rehabilitation plan to optimise recovery and minimise the risk of complications.
The recovery process involves a gradual return to normal activities. Physical therapists may prescribe specific exercises to improve joint mobility and strength. Patients are advised to follow the recommended rehabilitation plan to optimise recovery and minimise the risk of complications.
Prevention
Preventive measures focus on joint protection, ergonomic practices, and timely medical intervention. By incorporating these strategies into daily life, individuals can mitigate the risk of developing ganglion cysts and address potential issues at their early stages, enhancing overall joint health and well-being.
Avoidance of repetitive activities leading to irritation
Prevention involves avoiding repetitive activities that may lead to joint or tendon irritation. Identifying tasks that contribute to overuse or strain and implementing strategies to reduce such activities can play a crucial role in preventing the formation of ganglion cysts.
Proper ergonomics and joint-friendly practices
Implementing proper ergonomics in daily activities can contribute to joint protection. Using ergonomic tools and maintaining good posture helps reduce joint stress, minimising the risk of irritation and developing ganglion cysts. Joint-friendly practices promote overall joint health.
Seeking medical attention for new lumps or joint discomfort
Early intervention is key to preventing complications associated with ganglion cysts. Individuals who notice new lumps or experience joint discomfort should seek prompt medical attention. Timely evaluation allows for accurate diagnosis and appropriate management, potentially preventing the cyst from progressing or causing more significant issues.
Prompt diagnosis and management to prevent complications
Seeking medical attention at the onset of symptoms facilitates prompt diagnosis and management. Early intervention may involve conservative measures or minimally invasive procedures, preventing complications and reducing the likelihood of persistent symptoms or recurrence.
Importance Of Early Diagnosis And Intervention
Don’t hesitate to consult an orthopaedic specialist if you notice new lumps, experience joint discomfort, or have concerns about your musculoskeletal health. By taking proactive steps and partnering with medical professionals, you can navigate the journey to a healthier, more comfortable life. Your commitment to seeking timely advice is a vital investment in your long-term joint health and overall well-being.